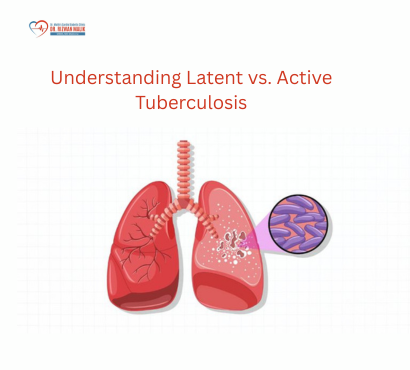
Understanding Latent vs Active Tuberculosis: What Patients Should Know
Tuberculosis (TB) is still one of the most important infectious diseases in India, but not everyone who has TB germs in the body is actually “suffering from TB.” Some people have latent TB, where germs are sleeping and cause no symptoms, while others have active TB, where germs are multiplying and making them sick. People often get confused between these two stages, worry about infection risk, and are unsure why doctors sometimes treat even when there are no symptoms. This guide explains the difference between latent and active TB in simple language, how each is diagnosed and treated, and what patients and families in India need to know to protect themselves and others. What Is Tuberculosis (TB)? TB is an infectious disease caused by the bacterium Mycobacterium tuberculosis. It most commonly affects the lungs (pulmonary TB) but can also involve lymph nodes, spine, brain, kidneys, intestines, and other organs (extra‑pulmonary TB). TB spreads through the air when someone with active lung TB coughs, sneezes, laughs, or speaks, releasing tiny droplets. After germs enter the body, one of two things can happen: the immune system controls them (latent TB) or they grow and cause illness (active TB). Latent TB vs Active TB: The Core Difference Latent TB infection (LTBI) TB germs are present in the body but are inactive (sleeping). The immune system keeps them under control and walls them off. There are no symptoms, the person feels well, and cannot spread TB to others. Active TB disease TB germs are actively multiplying, damaging tissues. The person has symptoms (often slowly progressive) and may spread TB to others if the lungs or airways are involved. About 5–10% of people with latent TB will develop active TB at some point in life, with higher risk in those with weak immunity. Key Differences at a Glance Feature Latent TB Infection Active TB Disease Germ activity Present but dormant Actively multiplying and damaging tissues Symptoms None; person feels normal Usually present: cough, fever, weight loss, etc. Infectious to others No Often yes (especially with lung TB) Chest X‑ray Normal or minor changes Usually abnormal in pulmonary TB Sputum (mucus) test Negative for TB bacteria Often positive for TB bacteria Treatment goal Prevent future disease Cure current disease & stop spread What Exactly Is Latent TB? When someone inhales TB germs, the immune system tries to control them. If it succeeds, the germs remain “walled off” but alive inside the body. Characteristics: No cough, no fever, no weight loss. Person is not contagious. Only clue is a positive TB skin test or TB blood test. Chest X‑ray is usually normal and sputum tests are negative. Latent TB is common in countries with high TB burden like India; many healthy adults may carry TB germs unknowingly. What Is Active TB? Active TB means the germs have broken through immune control and are multiplying. This can happen soon after first infection or years later if immunity weakens. Common symptoms of active pulmonary TB (lungs): Cough lasting more than 2–3 weeks. Coughing up mucus or blood. Chest pain or pain when breathing/coughing. Fever, usually low‑grade, often worse in evenings. Night sweats (waking up with wet clothes or bedding). Loss of appetite and unexplained weight loss. Fatigue, weakness, and feeling generally unwell. Active TB outside the lungs (extra‑pulmonary TB) may cause: Swollen lymph nodes (neck, armpit, groin). Back pain, deformity (spinal TB). Headache, vomiting, confusion (TB meningitis). Abdominal pain, diarrhoea or swelling (intestinal TB). Urinary symptoms or blood in urine (kidney TB). People with any of these unexplained symptoms, especially with TB exposure or living in India, should be evaluated promptly. Who Is at Higher Risk of Developing Active TB from Latent TB? Only a minority with latent TB develop active disease; risk increases when immunity is weak. High‑risk groups include: People with HIV infection. Patients on long‑term steroids or other strong immune‑suppressing medicines (for cancer, transplants, autoimmune diseases). People with diabetes, chronic kidney disease, or severe malnutrition. Very young children and elderly persons. Smokers and heavy alcohol users. Close household contacts of someone with active pulmonary TB. In such people, doctors often strongly recommend preventive treatment for latent TB. How Are Latent and Active TB Diagnosed? Diagnosing Latent TB Doctors rely on: TB skin test (Mantoux test / tuberculin skin test) A small amount of purified protein (PPD) is injected under the skin. The size of swelling after 48–72 hours is measured. TB blood tests (interferon‑gamma release assays – IGRA) Measure immune response to TB proteins in a lab. If either test is positive and there are no symptoms, normal chest X‑ray, and negative sputum, the person is usually considered to have latent TB. Diagnosing Active TB To diagnose active TB, doctors look for evidence of disease, not just infection: Clinical symptoms – prolonged cough, fever, weight loss, etc. Chest X‑ray or CT scan – changes in lungs suggestive of TB. Sputum tests – Microscopy for acid‑fast bacilli. Culture (grows TB germs; confirms diagnosis, but takes weeks). Molecular tests (e.g., PCR‑based) that detect TB DNA and drug resistance. For extra‑pulmonary TB, samples from affected organs (lymph node biopsy, fluid tapping, etc.) may be tested. Why Treat Latent TB If There Are No Symptoms? Even though latent TB is silent, the germs can “wake up” later, especially when immunity drops. Treating latent TB: Greatly reduces the chance of developing active TB later in life. Is especially important in high‑risk individuals (HIV, close contacts, immunosuppressed). Helps reduce TB burden in the community over time Preventive treatment regimens are usually shorter and milder than full courses for active TB. Treatment: Latent TB vs Active TB Treatment of Latent TB Infection Uses 1 or 2 medicines for several months (exact regimen depends on guidelines and patient factors). Goal: kill sleeping germs before they cause disease. Taken under supervision with periodic tests to ensure safety (especially liver function). People must complete the full course, even though they feel completely normal. Treatment of Active TB Disease Requires